>> How is HEALTHSPAN® being developed?
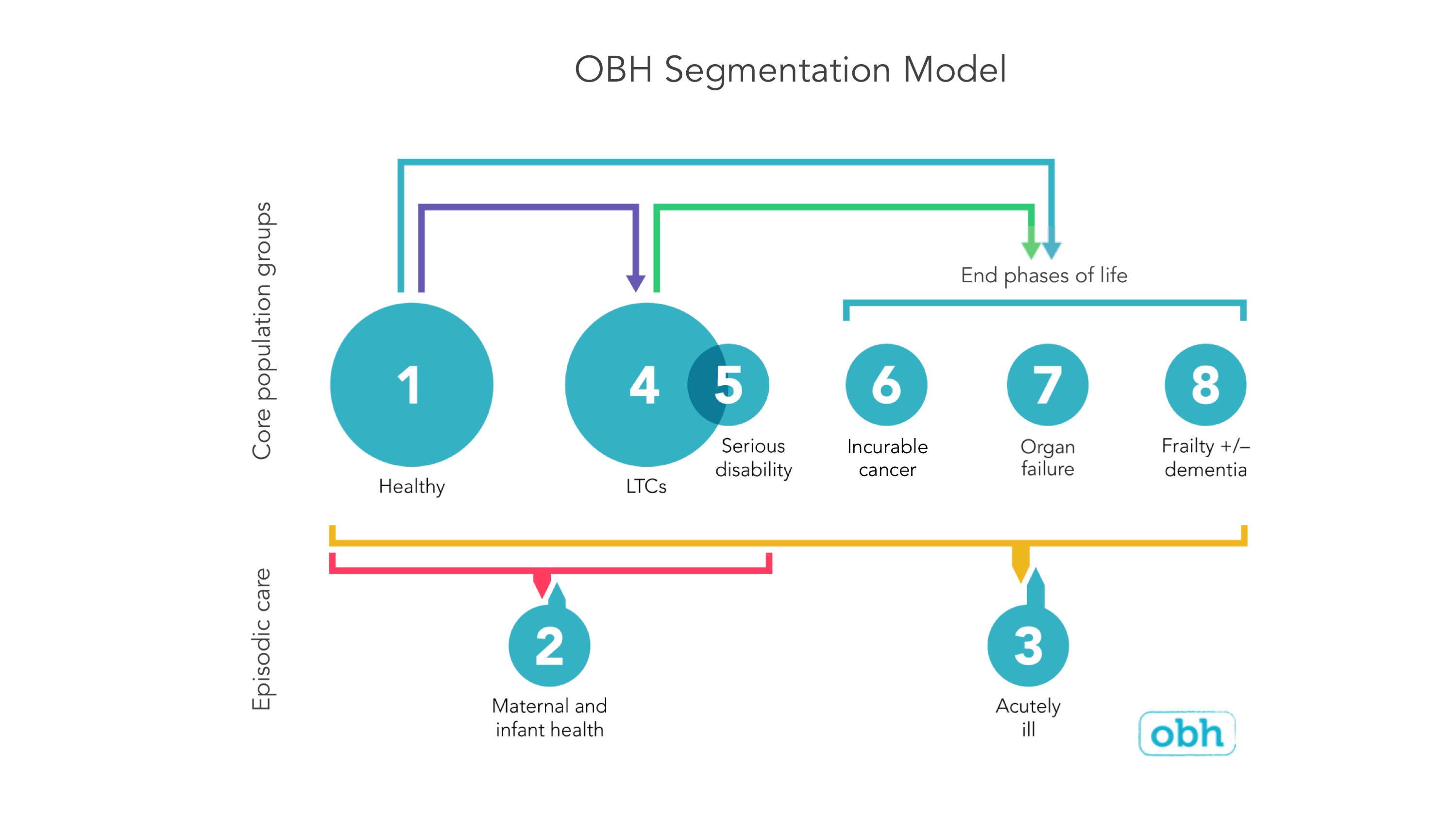
At OBH we have spent several years adapting the internationally recognised Bridges to Health segmentation model. We use this model for a whole population segmentation approach, to better understand population groups and how movement occurs within and between groups of people with broadly similar health and care needs. The currently healthy population segment is defined by exclusion from any other higher acuity segment (eg. like LTCs). Age groups can be added as required locally.
>> Why hasn’t this been done before?
This kind of data work requires substantial processing power. To analyse the dynamic nature of a population’s health, including the movement of people between population segments on a day-by-day basis, requires a very powerful, near-real-time model. With new technologies these technical barriers are being overcome all the time.
The groundwork to allow the calculation of HEALTHSPAN has also been extensive. An accurate definition of HEALTHSPAN is dependent upon a meticulously defined data model for all conditions that cause an individual to move out of the Healthy population segment. OBH’s work on the data-driven version of the Bridges to Health population segmentation model in recent years has involved the development of algorithms to define the most granular conditions and sub-conditions within each segment. With extensive clinical and data expertise these algorithms are now advanced to a point that allows highly reliable identification of people who are currently mostly healthy. Accurate calculation of HEALTHSPAN is tied to the quality of the overall population segmentation model being used.
>> What about improving the health of people who are already experiencing poor health?
The amount of time that people spend in good health is something that is currently not being measured in an objective and comprehensive way, which is why it is the primary focus of this new suite of measures. It is important, however, to also highlight that ‘health’ and ‘severity of ill-health’ can be measured across everyone in the population (not only people who are currently healthy).
The severity of chronic conditions, and the impact they have on a person’s life, varies greatly. In the same way that it is possible to identify the point at which people experience their first episode of poor health, the wider suite of measures also places emphasis on delaying and preventing the progression of long term conditions.
The OBH data-driven version of the Bridges to Health population segmentation model, provides a view of severity within each segment, and progression through different severity levels (e.g. based on stages of conditions, multi-morbidity, and other factors). This allows for evaluation of the success of secondary prevention (delaying/preventing the progression of a condition), as well as primary prevention (delaying/preventing the condition in the first place).
With the suite of HEALTHSPAN measures, the aim is to ensure that every individual in the population spends as much time in as good health as possible, whether or not they already have a chronic condition.
>> Isn’t HEALTHSPAN measured already?
There are a number of similar existing measures that have been used for a long time, including life expectancy, healthy life expectancy, QALYs and DALYs, amongst others. When compared with these other measures, HEALTHSPAN is the only metric that precisely measures the amount of time people spend in good health, in an objective, data-driven way, representing a whole population. Read more about comparisons with other measures.
>> Doesn’t the NHS know this already?
Whilst there are various sources of publicly available data related to the number of people with specific chronic conditions, frailty and disability in each area, these are usually from the perspective of a single condition, rather than the individual (who may have more than one condition). For example, the primary care Quality and Outcomes Framework (QOF) provides data on the number of people with a range of conditions, but because the overlaps between people on multiple disease registers are unknown, it is not possible to derive the number of people who do not have any of these conditions.
The precise proportion of the population who are healthy is therefore not known nationally, and without knowing who is currently healthy, it is impossible to calculate the HEALTHSPAN. This is new information for the NHS.
Similar existing measures to HEALTHSPAN, things like Healthy Life Expectancy, and Disability Adjusted Life Expectancy, are already reported nationally and locally, but these are based on self-reported health, or absence of limiting and long-standing illness or disability, from relatively small survey samples. The NHS does not know objectively from these how long everyone in the population is spending in good health.
>> We can now measure people's HEALTHSPANs. So what?
A measure is only useful if it provides an actionable insight. So once an area knows what their HEALTHSPAN is, what can they do about it?
The aim is of course to increase HEALTHSPAN (by more than the increase in lifespan, to ensure that people are spending more of their lives in good health), which will give people more years of good health, and simultaneously save the NHS money.
The OBH suite of HEALTHSPAN measures will guide people through the local reasons why people are first entering a period of significant poor health (e.g. the conditions that most commonly account for this, or inequalities in HEALTHSPAN by deprivation group). The next step is then to match evidence-based interventions to prevent and delay the onset of conditions to the high-risk groups identified for HealthSpan.
Previously it may have been difficult to measure the impact of these interventions locally. HEALTHSPAN makes this impact quantifiable, and therefore makes it easier for organisations to make the business case to implement these interventions. The case for prevention becomes much more tangible, at a whole population level.
The success of these interventions can then be monitored on an ongoing basis, in near-real time, to give rapid visibility of progress, and ensure that best use is being made of resources locally.
Subscribe to our Newsletter